Seizures in teens happen when there’s abnormal electrical activity in the brain, causing a variety of physical and mental symptoms. These episodes differ in how they look and how severe they are, impacting daily life and overall functioning.
The main symptoms of seizures in adolescents include convulsions, loss of consciousness, tingling sensations, or altered awareness, which are distressing for teens and their parents who witness these episodes. Teens with epilepsy face a higher risk of anxiety and depression due to the unpredictability of seizures. In North Carolina, more than 10% of children aged three to 17 were diagnosed with mood disorders such as depression or anxiety in 2020, marking a 49% rise since 2016.
The causes of seizures in teens include provoked factors you identify (like fever, head injuries, infections, or substance use) and unprovoked factors affecting you or your teen (such as genetic conditions, brain abnormalities, or previous neurological damage).
There are two main types of seizures: generalized seizures, which affect both sides of the brain, and focal seizures, which start in one specific area.
Diagnosis involves medical history, physical exams, EEG tests, and imaging like MRI or CT scans to identify brain abnormalities; parents play a key role by staying involved in the process.
Treatment includes antiepileptic medications, which reduce seizure frequency and intensity in about 70% of teens, per WHO 2024 research, while lifestyle changes and alternative treatments like ketogenic diets or surgery also improve outcomes.
What is a Seizure?
A seizure is a sudden, uncontrolled electrical disturbance in the brain that causes changes in behavior, movements, feelings, and consciousness. Seizures vary in duration and severity, with some lasting only a few seconds while others last several minutes. Worldwide, over 11 million children under the age of 15 are affected by epilepsy. In the United States, approximately 400,000 children have this condition, per research Gebeyaw B., et al published in BMC Public Health in 2024 titled “Prevalence, incidence, and trends of epilepsy among children and adolescents in Africa: a systematic review and meta-analysis.”
Seizures also lead to mental health disorders; children with epilepsy are at a higher risk of developing conditions such as anxiety and depression. The prevalence of depression among these children and adolescents remains notably high, ranging from 5.2% to 39.6%, as indicated in a study by Maryam S., et al published in the Iranian Journal of Pediatrics in 2013 titled “Depression in Children and Adolescents with Epilepsy: a 15 Year Research Review of Prevalence, and Demographic and Seizure Related Correlates.”
What Is The Difference Between A Seizure And Epilepsy?
The difference between a seizure and epilepsy is that a seizure is a single episode of abnormal electrical activity in the brain, which occurs due to various triggers, while epilepsy is a chronic neurological condition characterized by a tendency to have recurrent seizures. In other words, someone experiences a seizure without having epilepsy, but a diagnosis of epilepsy requires multiple unprovoked seizures over time.
What Are The Symptoms Of A Seizure In Teens?
The symptoms of seizures in teens are convulsions, loss of consciousness, tingling sensations, visual disturbances, and altered awareness. These symptoms are varied and affect the daily lives and mental health of teens.

The common symptoms of seizures include:
- Convulsions: Convulsions involve uncontrolled shaking and muscle spasms that last from seconds to minutes. If you’re witnessing this, it’s natural to feel alarmed or unsure of what to do. Staying calm allows you to support the person affected in the best way possible.
- Loss of consciousness: Loss of consciousness happens when a teen becomes unresponsive and doesn’t remember the episode later. For you as a parent or friend, this is understandably worrying. Watching someone go through this leaves you feeling confused or anxious about their well-being.
- Tingling sensations: Tingling sensations, like “pins and needles,” often occur before or during certain seizures. If you’re the one experiencing this, it might make you feel uneasy or signal that something isn’t right. Paying attention to these sensations helps you prepare for what’s ahead.
- Visual disturbances: Visual disturbances, such as seeing flashing lights or spots, are disorienting and act as warning signs. When you notice these changes, it’s a clear indication that a seizure might be coming. These moments can feel frightening, but understanding them helps reduce fear and uncertainty.
- Altered awareness: During a seizure, a teen may seem dazed or confused, losing track of their surroundings or conversations. If you’re with them, you’ll notice they struggle to communicate or engage with others. This affects their social interactions and relationships. For you as a parent or friend, offering patience and understanding helps them feel supported and less isolated.
What Are The Stages Of A Seizure?
The stages of a seizure are prodrome, aura, ictal, and postictal. Each phase plays a crucial role in the overall experience of a seizure.
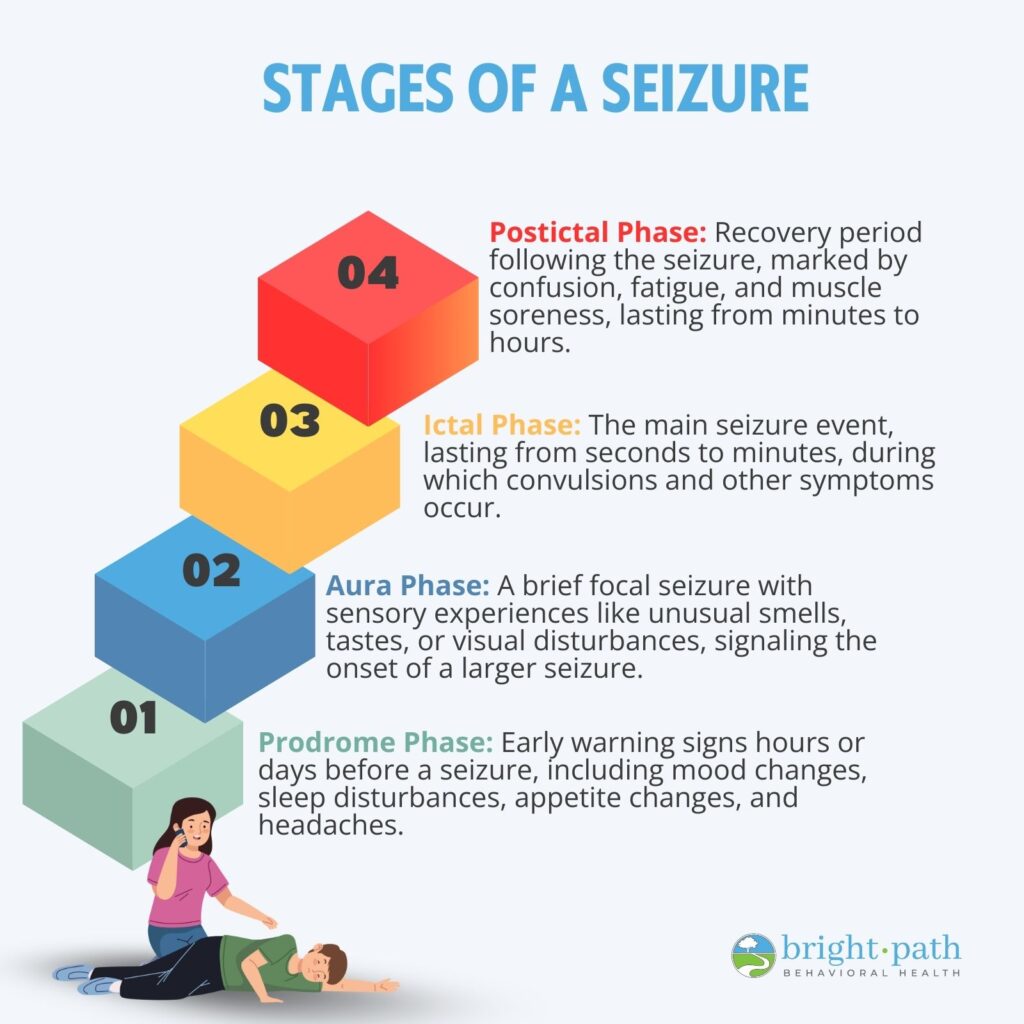
The stages of a seizure are listed below:
- Prodrome Phase: The prodrome phase begins hours or even days before the seizure occurs. Symptoms vary from person to person, and they serve as early warning signs that a seizure is imminent. Common symptoms in this phase include Mood changes (e.g., irritability or anxiety), sleep disturbances, changes in appetite, and headaches.
- Aura Phase: The aura phase is considered a type of focal seizure that precedes the main seizure activity. It usually lasts a few seconds to a couple of minutes and includes various sensory experiences. Symptoms include unusual smells or tastes, visual disturbances (e.g., flashing lights), tingling sensations, and feelings of déjà vu.
- Ictal Phase: This is the actual seizure event, during which the individual experiences the main symptoms of the seizure. It lasts from a few seconds to several minutes.
- Postictal Phase: Following the seizure, the ictal phase involves recovery and lasts from several minutes to hours. Symptoms include confusion, fatigue, and muscle.
What Are The Warning Signs Of A Seizure?
The warning signs of a seizure in teens are sensory symptoms, emotional changes, and autonomic symptoms. These signs serve as important indicators that a seizure is approaching, although not everyone experiences them.

The warning signs of a seizure are listed below:
- Sensory Symptoms: Sensory symptoms of a seizure include unusual experiences like strange smells, tastes, or visual disturbances such as flashing lights. You might also feel tingling or numbness in your limbs. These signs often come before a seizure, giving you a chance to find a safe space or let someone nearby know what’s happening.
- Emotional Changes: Emotional changes happen when teens suddenly feel anxious, fearful, or irritable without a clear reason. You might also experience déjà vu (feeling like you’ve been through this moment before) or jamais vu (feeling like something familiar is strange). These shifts are confusing and distressing, but recognizing them helps you prepare for what’s coming next.
- Autonomic Symptoms: Autonomic symptoms involve changes in your body’s involuntary functions, like a racing heart, excessive sweating, or nausea. If you’re noticing these signs, it means your nervous system is reacting to an upcoming seizure. Understanding these symptoms allows you and those around you to respond in a way that keeps you safe and supported.
What Are The Causes Of A Seizure In Teens?
The causes of seizures in teens are provoked and unprovoked seizures. Provoked seizures occur in response to specific triggers, such as illness or environmental factors, while unprovoked seizures arise without an identifiable cause and indicate an underlying neurological condition.
The causes of seizures are detailed below:
Provoked Seizures
Provoked seizures are those that happen due to specific factors or triggers. These seizures are temporary and resolve once the underlying cause is addressed. Common causes of provoked seizures in teens include:
- Febrile Illness: High fever, especially in younger individuals, leads to seizures known as febrile seizures. These are usually seen in children under five but occur in teens during severe infections. Approximately 30% of children with one febrile seizure will experience another, per a review by Rana S., et al published in Frontiers in Pediatrics in 2022 titled “A Review of Febrile Seizures: Recent Advances in Understanding of Febrile Seizure Pathophysiology and Commonly Implicated Viral Triggers.”
- Head Trauma: Injuries to the head, whether from accidents or sports, disrupt normal brain activity and trigger seizures. It accounts for around 10-20% of new-onset seizure cases in adolescents, according to research published in Science Direct in 2015 titled “Traumatic brain injury and epilepsy: Underlying mechanisms leading to seizure.” The risk is particularly high if the injury causes bleeding or swelling in the brain.
- Infections: Conditions such as meningitis (inflammation of the brain’s protective membranes) or encephalitis (inflammation of the brain itself) lead to seizures. These infections cause significant neurological damage and require immediate medical attention.
- Substance Abuse: Withdrawal from drugs or alcohol provokes seizures due to chemical imbalances in the brain. This is particularly common in individuals with a history of substance dependency. Withdrawal seizures occur in roughly 5-10% of individuals with alcohol dependency, within 6-48 hours after the last drink, per a 2022 study published in Science Direct titled “Alcohol Withdrawal Seizure.”
- Metabolic Imbalances: Abnormal levels of electrolytes (like sodium or potassium), glucose, or other bodily substances lead to seizures. Conditions such as diabetic ketoacidosis or kidney failure result in such imbalances.
- Sleep Deprivation: Lack of adequate sleep lowers the seizure threshold in susceptible individuals. Sleep plays a crucial role in brain function, and chronic deprivation leads to neurological disturbances.
- Medication Non-compliance: Missing doses of prescribed anti-seizure medications lead to breakthrough seizures. Consistency in taking medication is vital for managing seizure disorders effectively.
- Exposure to Toxins: Environmental toxins, such as lead or carbon monoxide, provoke seizures by disrupting brain function. This exposure requires immediate removal from the environment and medical intervention.
Unprovoked Seizures
Unprovoked seizures occur without any identifiable external triggers and usually indicate an underlying neurological disorder. These seizures are part of a chronic condition like epilepsy. Common causes of unprovoked seizures include:
- Epilepsy: A chronic neurological disorder characterized by recurrent, unprovoked seizures. It varies in severity and frequency, requiring long-term management.
- Genetic Factors: A family history of seizure disorders increases the risk of unprovoked seizures in teens. Certain genetic mutations and syndromes are linked to a higher likelihood of developing epilepsy. A population-based study by Anna L., et al published in the Brain in 2014 titled “Familial risk of epilepsy” found that the cumulative incidence of epilepsy among relatives of affected individuals by age 40 was 4.7%, representing a 3.3-fold increase compared to the general population. The highest risks were seen in relatives of those with idiopathic generalized epilepsies (standardized incidence ratio of 6.0) and those with prenatal or developmental causes (ratio of 4.3).
- Brain Malformations: Abnormalities in brain structure, whether congenital or acquired, lead to unprovoked seizures. These malformations disrupt normal electrical activity in the brain.
- Cerebral Palsy: This neurological condition, resulting from brain development issues, includes seizure activity. Seizures in individuals with cerebral palsy vary in type and frequency. Seizures occur in approximately 30-50% of individuals with cerebral palsy, as mentioned in an analysis published by the Cerebral Palsy Guide titled “Cerebral Palsy and Epilepsy”
- Stroke: Reduced blood flow to the brain, due to a clot or hemorrhage, triggers unprovoked seizures. This is particularly concerning in teens with conditions that increase stroke risk. In a 2017 study by Tomas B. et al., published in the “Journal of Stroke and Cerebrovascular Diseases,” early seizures (ES) occurring within 24 hours to 30 days after an ischemic stroke were reported in 1.8% to 16.6% of cases. Late seizures (LS), which develop after this early period, occur in about 3% to 7.3% of stroke survivors.
- Tumors: Brain tumors disrupt normal electrical activity and provoke unprovoked seizures. Depending on the tumor’s location and type, seizures vary significantly in their presentation.
- Neurodegenerative Diseases: Conditions that cause progressive brain degeneration, such as multiple sclerosis or Alzheimer’s disease, lead to unprovoked seizures. These diseases affect cognitive and physical functions over time, including seizure thresholds. Unprovoked seizures occur in about 10 to 22% of individuals with neurodegenerative diseases, such as Alzheimer’s disease, as the brain’s electrical activity becomes disrupted, according to a study by Keith A., et al published in the Lancet Neurol in 2017 titled “Epileptic activity in Alzheimer’s disease: causes and clinical relevance.”
- Previous Head Injuries: Past concussions or significant head trauma result in unprovoked seizures later in life. The brain remains sensitive to seizure triggers long after the initial injury has healed.
What Are The Risk Factors For a Seizure?
The risk factors for a seizure include a family history of seizures, age under 18 years, head or brain injuries, cognitive issues, and Alzheimer’s disease.

The common risk factors for seizure include:
- Family history of seizures: A genetic predisposition significantly increases the likelihood of seizures, as certain types of epilepsy run in families, suggesting a hereditary component. A 2014 population-based study by Anna L. et al., published in Brain and titled “Familial Risk of Epilepsy,” found that the cumulative incidence of epilepsy among relatives of affected individuals by age 40 was 4.7%, a 3.3-fold increase compared to the general population. The highest risks were among relatives of individuals with idiopathic generalized epilepsies (standardized incidence ratio of 6.0) and those with prenatal or developmental causes (ratio of 4.3).
- Age under 18 years: Adolescents are more prone to seizures due to ongoing brain development, which leads to increased neuronal excitability and susceptibility to seizure activity.
- Head or brain injuries: Trauma to the head, such as concussions or more severe brain injuries, disrupt normal brain function and trigger seizures, particularly if there is damage to the cerebral cortex.
- Cognitive issues: Conditions that affect cognitive function, such as learning disabilities or intellectual disabilities, disrupt neural pathways, making individuals more vulnerable to seizures.
- Alzheimer’s disease: Although it primarily affects older adults, early-onset Alzheimer’s leads to seizures due to neurodegeneration and changes in brain structure, which affect electrical activity in the brain. 10 to 22% of individuals with neurodegenerative diseases like Alzheimer’s disease experience disrupted brain electrical activity, as mentioned in a study by Keith A. et al., published in Lancet Neurology in 2017, titled “Epileptic Activity in Alzheimer’s Disease: Causes and Clinical Relevance.”
What Are The Types Of a Seizure?
The types of seizures in teens are generalized seizures and focal seizures. Generalized seizures involve both hemispheres of the brain, leading to widespread symptoms such as loss of consciousness. In contrast, focal seizures originate in a specific area of the brain, causing localized effects that vary based on the region affected.
The types of a seizures include:
Generalized Seizures
Generalized seizures occur when abnormal electrical activity affects both sides of the brain, resulting in a loss of consciousness. The types of generalized seizures include:
- Tonic-Clonic Seizures: Characterized by stiffening of the body (tonic phase) followed by rhythmic jerking (clonic phase).
- Absence Seizures: Brief episodes of staring or unresponsiveness, lasting just a few seconds.
- Myoclonic Seizures: Sudden, brief jerks or twitches of a muscle or muscle group.
- Atonic Seizures: Sudden loss of muscle tone, causing the person to collapse or fall.
- Clonic Seizures: Repetitive jerking movements, affecting the limbs.
Focal Seizures
Focal seizures, also known as partial seizures, begin in a specific area of the brain and affect consciousness to varying degrees. The types of focal seizures include:
- Focal Aware Seizures: The person remains conscious and aware, experiencing unusual sensations or movements.
- Focal Impaired Awareness Seizures: The individual has altered consciousness and does not respond to stimuli, displaying automatic behaviors.
- Focal to Bilateral Tonic-Clonic Seizures: This starts as a focal seizure and spreads to both sides of the brain, resulting in a tonic-clonic seizure.
How is a Seizure Diagnosed?
A Seizure is diagnosed through a comprehensive process that includes a detailed medical history and neurological examination. To further investigate the underlying causes, a variety of laboratory tests are conducted, including imaging studies and electrical activity monitoring.

The following tests are used in the diagnostic process:
- Neurological exam: This evaluates cognitive function, reflexes, and motor skills.
- Blood tests: Blood tests check for metabolic or electrolyte imbalances, infections, and other underlying conditions.
- Spinal tap: The spinal tap analyzes cerebrospinal fluid for signs of infection or inflammation.
- Electroencephalogram (EEG): EEG helps to record electrical activity in the brain to identify abnormal patterns indicative of seizures.
- MRI: This provides detailed images of the brain to detect structural abnormalities.
- CT scan: CT scan Offers cross-sectional images of the brain to identify injuries or lesions.
- Positron emission tomography (PET): This assesses brain metabolism and function.
- Single-photon emission computerized tomography (SPECT): Measures blood flow in the brain to identify areas of abnormal activity.
Together, these diagnostic tools help healthcare providers determine the type of seizure and its potential causes, guiding effective treatment options.
How is a Seizure in Teens Treated in North Carolina?
In North Carolina, seizures in teens are treated through a combination of medication, surgery, vagus nerve stimulation, responsive nerve stimulation, and deep brain stimulation.
For teens struggling with seizure-related mental health challenges, we offer comprehensive mental health treatment that includes intensive outpatient programs, partial hospitalization, and virtual services. Our approaches incorporate family support while providing ongoing care for those needing additional support through our extended path program.
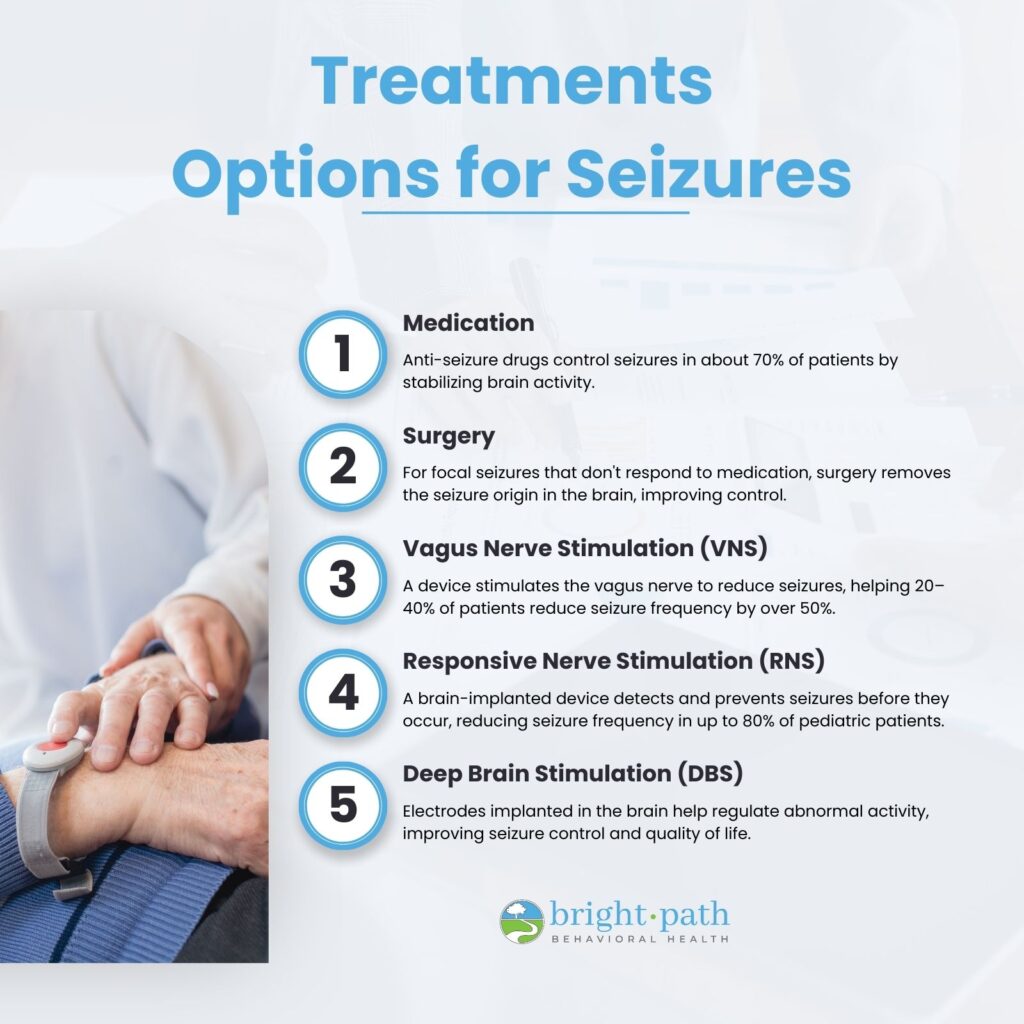
The treatments for seizures include:
- Medication: Anti-seizure drugs are prescribed to control seizures by stabilizing electrical activity in your brain. They are customized based on the type of seizures and how you respond to treatment. This approach reduces the frequency and severity of seizures.
- Surgery: Surgical interventions are considered for patients with focal seizures who do not respond to medication. The procedure involves removing the area of the brain where seizures originate. This treatment leads to significant improvements in seizure control and quality of life for eligible candidates.
- Vagus Nerve Stimulation (VNS): With VNS, a device is implanted to send electrical impulses to your vagus nerve, reducing seizure frequency and intensity by modulating brain activity. If medications don’t work well for you, VNS can be particularly beneficial. VNS is particularly beneficial for you if you do not respond well to medications. Research from a 2012 review in the Surgical Neurological International Journal shows that about 20–40% of patients experience over a 50% reduction in seizure frequency with VNS therapy. Response rates tend to improve over time, and you may need fewer anti-epileptic drugs after starting VNS.
- Responsive Nerve Stimulation (RNS): An RNS device is implanted in your brain to monitor for seizure activity and deliver electrical stimulation when it detects an impending seizure. This proactive approach prevents seizures before they happen and is especially helpful if you have drug-resistant epilepsy. Approximately 80% of pediatric patients reported more than a 50% reduction in seizures with RNS therapy, as stated in the study titled “Responsive Neurostimulation for Drug-Resistant Epilepsy.”
- Deep Brain Stimulation (DBS): DBS involves placing electrodes in specific areas of your brain to deliver continuous electrical impulses. This treatment modulates abnormal brain activity linked to seizures, improving seizure control and overall quality of life for some patients.
How to Prevent Seizures in Teens of North Carolina?
To prevent seizures in teens, it’s essential to ensure medication compliance, maintain a regular sleep schedule, manage stress, avoid triggers, follow a healthy diet, and attend regular checkups.
Some effective tips and strategies for preventing seizures include:
- Medication Compliance: Take prescribed anti-seizure medications regularly and exactly as directed by a healthcare provider. Sticking to this routine supports your health and seizure management.
- Regular Sleep Schedule: Keep a consistent sleep routine. Fatigue and sleep deprivation lead to seizures, so prioritizing rest helps you stay balanced.
- Stress Management: Practice stress-reducing activities like yoga, meditation, or deep-breathing exercises. Lowering anxiety levels reduces the likelihood of seizures.
- Avoiding Triggers: Identify and steer clear of known seizure triggers such as flashing lights, specific sounds, or certain foods. Awareness of these factors keeps you safer.
- Healthy Diet: Follow a balanced diet and stay hydrated. Some individuals benefit from a ketogenic diet, but discussing this with a healthcare professional ensures it’s right for you.
- Limit Alcohol and Caffeine: Cut back on alcohol and caffeine, as both disrupt seizure control. Making these changes supports your overall well-being.
- Regular Check-ups: Schedule consistent appointments with a healthcare provider. Monitoring epilepsy management allows for adjustments to treatments and keeps you on track.
How Long Do Seizures Last?
Most seizures last between 30 seconds to 2 minutes. However, some focal seizures are shorter, lasting only a few seconds, while generalized seizures extend beyond 2 minutes. If a seizure lasts longer than 5 minutes or if multiple seizures occur in succession without recovery, it is considered a medical emergency, and immediate medical attention is required.
Can You Die From A Seizure?
Yes, it is possible to die from a seizure, although such occurrences are rare. The phenomenon known as Sudden Unexpected Death in Epilepsy (SUDEP) is a significant concern for individuals with epilepsy. SUDEP occurs in approximately 1 in 1,000 adults with epilepsy each year, and the risk is even lower in children, estimated at 1 in 4,500, according to research by CDC in 2024 titled “Sudden unexpected death in epilepsy.” Most SUDEP cases happen during generalized seizures, while the person is asleep.
Do Seizures Cause Brain Damage?
Yes, seizures cause brain damage, particularly in cases of prolonged or severe seizures. While brief seizures do not result in significant neuronal death, more intense and repetitive seizures, such as those seen in status epilepticus, are known to lead to substantial neuronal loss and brain injury.
Status epilepticus causes extensive damage in vulnerable brain regions, with studies by Ray D., et al published in the Advances in Experimental Medicine and Biology in 2014 titled “When and How Do Seizures Kill Neurons, and Is Cell Death Relevant to Epileptogenesis?” showing that up to 20-40% of patients develop cognitive impairments following episodes of status epilepticus. Also, the immature brain is more resistant to the long-term effects of seizures, but prolonged seizures still lead to lasting neurological consequences. The relationship between seizures and brain damage remains complex, with ongoing debates about the mechanisms involved and the extent of damage caused by different types of seizures.
Can Seizures Cause Mental Health Issues?
Yes, seizures can cause mental health issues. A meta-analysis by Marco M., et al published in Neurology Clinical Practice in 2021 titled “Psychiatric Comorbidities in People With Epilepsy” found that the prevalence of active depression in adults with epilepsy is 23.1%, significantly higher than in the general population. Anxiety disorders also show a pooled prevalence of 20.2% among those with epilepsy. The relationship between seizures and mental health issues is bidirectional.
Can Lack Of Sleep Trigger A Seizure?
Yes, a lack of sleep triggers a seizure. Sleep deprivation is recognized as a significant risk factor for seizure occurrence, particularly in individuals with epilepsy and sleep disorders. About 60% of patients with epilepsy reported that sleep deprivation was a seizure trigger for them, as mentioned in research by Maurine M., et al published in Science Direct in 2015 titled “Impact of sleep duration on seizure frequency in adults with epilepsy: A sleep diary study.” The underlying mechanisms involve alterations in neurotransmitter systems and increased neuronal excitability due to insufficient restorative sleep. Therefore, maintaining a regular sleep schedule is essential for individuals prone to seizures.