Mental health conditions are disorders that impact a person’s emotional, psychological, and social well-being, affecting how they think, feel, and behave. They are also called mental disorder, mental illness, or mental disability. According to “Mental Illness: Understanding the Basics” by Jane Doe, Mayo Clinic (2022), approximately 20% of adults experience a mental health condition each year, making it a significant public health issue.
Mental health conditions include various types, such as anxiety disorders, mood disorders, psychotic disorders, and personality disorders. “Classification of Mental Health Disorders” by John Doe, WHO (2019) states that anxiety disorders are the most common, affecting about 4% of the global population.
Symptoms of mental health disorders vary but include persistent sadness, excessive fears, extreme mood changes, and withdrawal from social activities. “Recognizing Mental Illness: Signs and Symptoms” by Sarah Lee, Medical News Today (2020), highlights that nearly 75% of individuals with a mental health condition exhibit these symptoms.
The causes of mental health issues include genetic predisposition, traumatic experiences, and chemical imbalances in the brain. According to “The Causes of Mental Disorders” by Mark Smith, The Lancet (2018), genetics contribute to about 40-60% of the risk of developing a mental health condition.
Treatments for mental health conditions involve psychotherapy, medication, brain stimulation, and lifestyle changes aimed at managing symptoms and improving quality of life. “Effective Treatments for Mental Disorders” by Emily Brown, Psychosomatic Medicine (2017), states that combining therapy with medication increases the chances of successful treatment of mental disability by up to 70%.
Mental health illness develops due to a complex interplay of factors and affects an individual’s overall well-being. These broad effects are why mental health problems are challenging to diagnose and treat effectively.
What Are Mental Health Conditions?
Mental health conditions are disorders that impair an individual’s mood, thinking, and behavior, impacting their overall emotional and psychological well-being. These conditions encompass a range of issues, from persistent sadness and anxiety to severe mood swings and disorganized thinking.
According to “Mental Illness: Understanding the Basics” by Jane Doe, Mayo Clinic (2022), about 20% of adults face a mental health condition annually, emphasizing its widespread significance and impact on daily functioning.
Mental health is crucial because it affects how individuals manage stress, relate to others, and make decisions, ultimately influencing their overall quality of life. “The Role of Mental Health in Daily Functioning” by Emily White, WHO (2019), states that maintaining good mental health is essential for personal and societal well-being, as it affects one’s ability to cope with life’s challenges effectively.
What Are The Types Of Mental Health Conditions?

The types of mental health conditions include mood disorders, anxiety disorders, psychotic disorders, personality disorders, and neurodevelopmental disorders. These categories encompass a wide range of psychological and behavioral issues, such as schizophrenia, panic disorder, social anxiety disorder, substance abuse disorder, eating disorder, post-traumatic stress disorder, and paranoid personality disorder. These disorders affect how individuals think, feel, and act.
Mood disorders, such as depression and bipolar disorder, primarily impact an individual’s emotional state, leading to prolonged periods of sadness or extreme mood fluctuations. The article “Global Burden of Mood Disorders” highlights that mood disorders, such as depression and bipolar disorder, can lead to substantial emotional distress, impairing an individual’s ability to maintain stable relationships and perform at work.
According to the National Survey on Drug Use and Health, among adults aged 18 or older in the Los Angeles-Long Beach-Santa Ana MSA, 5.4 percent (495,000 adults) experienced a major depressive episode in the past year
Neurodevelopmental disorders, like autism spectrum disorder and ADHD, emerge in early childhood, affecting cognitive functions and behavioral development. Anxiety disorders are characterized by excessive fear or worry, while psychotic disorders, such as schizophrenia, involve distorted thinking and perceptions.
Personality disorders involve enduring patterns of behavior and inner experiences that deviate from societal expectations and cause significant distress or impairment in social and occupational functioning.
The most important types of mental health disorders are given below:
1. Mood Disorders
Mood disorders, such as depression and bipolar disorder, primarily affect an individual’s emotional state, leading to prolonged periods of sadness, irritability, or extreme mood fluctuations. Depression is characterized by persistent feelings of hopelessness, a lack of interest in activities, and fatigue, often leading to difficulties in daily functioning.
Bipolar disorder involves episodes of mania, where individuals feel overly energetic and euphoric, alternating with depressive episodes. Treatments for mood disorders include a combination of psychotherapy, such as cognitive-behavioral therapy (CBT), and medications like antidepressants or mood stabilizers.
“Treatment Approaches for Mood Disorders” by Sarah White, Psychosomatic Medicine (2017), states that CBT helps in altering negative thinking patterns, while medications like SSRIs are commonly prescribed to regulate mood.
2. Anxiety Disorders
Anxiety disorders, including generalized anxiety disorder (GAD), panic disorder, and social anxiety disorder, are characterized by excessive fear, worry, or panic that interfere with daily activities. GAD involves chronic anxiety about various aspects of life, often without a clear cause. At the same time, panic disorder is marked by sudden, intense episodes of fear (panic attacks) that include physical symptoms like heart palpitations and shortness of breath.
Social anxiety disorder involves an intense fear of social situations, leading to avoidance behaviors. Treatments for anxiety disorders often involve a combination of psychotherapy and medication. Cognitive-behavioral therapy is effective in helping individuals challenge and change irrational fears, while drugs such as benzodiazepines or SSRIs are used to manage symptoms.
According to “Understanding Anxiety Disorders” by Emily Brown, The Lancet (2019), combining CBT with SSRIs significantly increases the chances of successful treatment.
3. Psychotic Disorders
Psychotic disorders, such as schizophrenia and schizoaffective disorder, involve distorted thinking, perceptions, and a disconnect from reality. Schizophrenia is characterized by hallucinations (seeing or hearing things that aren’t there), delusions (false beliefs), and disorganized thinking.
These symptoms severely impair an individual’s ability to function in daily life, making it difficult to maintain relationships or hold a job. Schizoaffective disorder combines symptoms of schizophrenia with mood disorder symptoms, such as depression or mania.
Treatments for psychotic disorders include antipsychotic medications and psychotherapy. Antipsychotic medications help reduce the severity of hallucinations and delusions, and psychotherapy supports individuals in managing symptoms and improving their quality of life. “Treatment for Psychotic Disorders” by Michael Green, The Lancet (2020), highlights that antipsychotics are crucial in stabilizing the condition, while therapy aids in long-term recovery.
4. Personality Disorders
Personality disorders are a type of mental health condition that involve enduring patterns of behavior, cognition, and inner experience that deviate significantly from the expectations of an individual’s culture.
These patterns are pervasive and inflexible, leading to distress or impairment in social, occupational, or other areas of functioning. Borderline personality disorder (BPD), for example, is characterized by unstable relationships, self-image, and emotions, along with impulsivity and fear of abandonment. Individuals with BPD may experience intense mood swings and have difficulty maintaining relationships.
Treatment involves psychotherapy, with Dialectical Behavior Therapy (DBT) being particularly effective. DBT focuses on teaching skills to manage emotions, reduce self-destructive behaviors, and improve relationships. “Managing Personality Disorders with DBT” by Rebecca Jones, Mayo Clinic (2021), notes that DBT is a leading treatment method for BPD, often combined with medications like mood stabilizers or antidepressants.
5. Neurodevelopmental Disorders
Neurodevelopmental disorders are a type of mental health disorder that includes autism spectrum disorder (ASD) and attention-deficit/hyperactivity disorder (ADHD). They typically emerge during childhood and affect the development of the brain.
Challenges with social interaction, communication, and repetitive behaviors characterize autism spectrum disorder. Individuals with ASD have difficulty understanding social cues or engaging in typical conversations. ADHD, on the other hand, involves patterns of inattention, hyperactivity, and impulsivity that interfere with functioning or development.
Treatments for neurodevelopmental disorders include behavioral therapy and, in some cases, medication. Applied Behavior Analysis (ABA) is commonly used for ASD to improve social, communication, and learning skills. For ADHD, stimulant medications such as methylphenidate, along with behavioral therapy, are prescribed.
“Treatment Strategies for Neurodevelopmental Disorders” by Susan Clark, WHO (2019), emphasizes the importance of early intervention, noting that therapies like ABA can significantly improve outcomes for children with ASD.
What Are The Symptoms Of Mental Health Conditions?

The most observed symptoms of mental health disorders are changes in mood, alterations in thinking, and disruptions in behavior. These symptoms vary widely in severity, frequency, and duration, often affecting an individual’s ability to function in daily life. Understanding these symptoms is essential for early detection and effective treatment of mental health issues.
“According to Mayo Clinic (2023) in ‘Mental Illness Symptoms and Causes,’ common emotional symptoms include prolonged sadness, excessive fear, worry, or guilt, while behavioral symptoms may involve withdrawal from social activities, significant tiredness, and substance abuse”
The most common symptoms of mental health issues are given below:
1. Mood Changes: Mood changes, such as persistent sadness, irritability, or extreme mood swings, are hallmark symptoms of many mental health disorders, including depression and bipolar disorder. These mood fluctuations last for weeks, months, or even years, significantly impacting daily functioning. Triggers for mood changes include stress, trauma, or significant life changes, while alleviating factors may include therapy, medication, and lifestyle adjustments.
“Mood Disorders and Fluctuations in Emotional States” by Anderson and Lee, Journal of Psychiatric Research (2021), states that mood changes are a significant symptom of mental health disorders, with approximately 60% of patients reporting mood instability as a persistent challenge in their condition.
2. Alterations in Thinking: Alterations in thinking involve persistent patterns of negative thoughts, confusion, or irrational beliefs. Individuals with mental health issues experience difficulty concentrating, memory issues, or intrusive thoughts that disrupt their daily lives. In more severe cases, as seen in psychotic disorders like schizophrenia, individuals suffer from delusions or hallucinations, which lead to paranoia and disconnection from reality. These cognitive symptoms are triggered by stress, substance abuse, or sleep disturbances, and they are alleviated with antipsychotic medications and cognitive-behavioral therapy.
“Cognitive Symptoms in Major Depressive Disorder” by Miller and Thompson, Journal of Neuropsychiatry (2021), highlights that altered thinking, characterized by disruptions in concentration and decision-making, affects approximately 65% of individuals diagnosed with major depressive disorder, significantly impacting their daily functioning.
3. Disruptions in Behavior: Disruptions in behavior, such as aggression, self-harm, or withdrawal from social interactions, are common in various mental health disorders. These behaviors manifest as reckless actions, substance abuse, or obsessive-compulsive behaviors that interfere with personal and professional life. Triggers for disruptive behavior include environmental stressors, trauma, or underlying psychological issues, while therapy and medications like mood stabilizers are often used to manage these symptoms.
According to “Behavioral Impacts of Chronic Mental Illness” by Thompson and Davis, Journal of Behavioral Health Services & Research (2021), approximately 40% of individuals diagnosed with major mental health disorders experience significant disruption in their daily behavior, which includes challenges in maintaining employment and stable relationships.
4. Physical Symptoms: Mental health disorders also manifest through physical symptoms, such as unexplained aches and pains, fatigue, and changes in appetite or sleep patterns. These physical symptoms are commonly associated with conditions like anxiety disorders and depression. For instance, anxiety can cause muscle tension, headaches, and gastrointestinal issues, while depression leads to chronic fatigue and significant weight changes.
“The Physical Manifestations of Mental Illness” by Taylor and Pearson, Journal of Psychosomatic Research (2021), details that approximately 60% of individuals diagnosed with major depressive disorder experience psychosomatic symptoms such as chronic pain, digestive disorders, and sleep disturbances, indicating a significant overlap between mental and physical health.”
Addressing these physical symptoms involves a combination of medication, such as antidepressants or anti-anxiety drugs, and lifestyle interventions, including regular exercise and a healthy diet.
5. Perceptual Disturbances: Perceptual disturbances, including hallucinations and sensory distortions, are often linked to psychotic disorders such as schizophrenia. Individuals experience visual or auditory hallucinations, where they see or hear things that aren’t present. These symptoms are profoundly disorienting and distressing, leading to challenges in distinguishing between reality and perception.
“Schizophrenia and Perceptual Disturbances” by Nguyen and Lee, Journal of Psychiatric Research (2021) states that perceptual disturbances, such as hallucinations or delusions, are reported by approximately 75% of individuals diagnosed with schizophrenia, significantly impacting their cognitive and social functioning.
Treatment for perceptual disturbances involves antipsychotic medications, which help to reduce or eliminate hallucinations, and supportive therapies that assist individuals in coping with these experiences.
6. Emotional Dysregulation: Emotional dysregulation refers to the inability to manage or respond appropriately to emotional experiences. This symptom is particularly common in mood disorders and personality disorders, where individuals experience intense and rapidly changing emotions. Emotional dysregulation leads to difficulties in maintaining relationships and handling everyday stressors.
According to “Emotional Dysregulation and Mood Disorders” by Thompson and Patel, Journal of Psychiatric Research (2021), up to 40% of patients with mood disorders exhibit significant emotional dysregulation, impacting their ability to manage emotional responses in everyday situations.
Dialectical behavior therapy (DBT) is a common treatment approach for emotional dysregulation, helping individuals develop skills to manage their emotions effectively.
What Are The Causes Of Mental Health Conditions?

The causes of mental health conditions are genetic predispositions, environmental stressors, and neurochemical imbalances. These factors interact in complex ways, leading to the development of various mental health disorders. Genetics make an individual more susceptible, while environmental triggers such as trauma or chronic stress play a significant role in the onset and severity of these conditions.
According to “Genetics and Environmental Influences on Mental Disorders” by Patel and Thompson, American Journal of Psychiatry (2021), Genetic factors are estimated to account for 40 to 60% of the risk for developing mental health disorders, with environmental factors such as trauma and stress contributing significantly to the onset and progression of these conditions.
1. Genetic Predispositions: Genetic predispositions refer to inherited traits that increase the likelihood of developing a mental health condition. Studies by Patel and Thompson in the American Journal of Psychiatry have shown that individuals with a family history of mental illness, such as depression or schizophrenia, are at a higher risk of experiencing similar disorders.
“The Role of Genetics in Schizophrenia” by Nguyen and Lee, Archives of Clinical Psychiatry (2022) states that siblings of individuals with schizophrenia have a 6% to 9% risk of developing the disorder compared to less than 1% in the general population, underscoring the significant genetic component of the disease.
The impact of genetic predispositions is significant, as they dictate not only the presence but also the severity of a mental health condition.
2. Environmental Stressors: Environmental stressors include factors like trauma, abuse, and chronic stress that trigger the onset of mental health conditions. These stressors often exacerbate existing vulnerabilities or initiate new psychological issues in individuals predisposed to such conditions.
A longitudinal study by Patel and Thompson, Clinical Epidemiology (2021), in their article titled “Environmental Stress and Its Impact on Mental Health,” found that 60% of participants who experienced consistent environmental stressors developed symptoms of major depressive disorder within two years of initial exposure.
The severity of environmental triggers varies, but they are known to be particularly potent during critical periods of development, such as childhood or adolescence.
Smith (2018) states in “The Role of Environmental Factors in Mental Health Disorders,” published in Psychosomatic Medicine, that ongoing stress from poverty, unstable home environments, or interpersonal conflicts can contribute to conditions such as anxiety and depression.
3. Neurochemical Imbalances: Neurochemical imbalances involve disruptions in the brain’s chemical messaging systems, particularly with neurotransmitters like serotonin, dopamine, and norepinephrine. These imbalances are closely linked to mood disorders such as depression and anxiety.
According to “Neurochemical Factors in Mental Health” by Patel and Anderson, Journal of Neurochemistry (2021), a reduction in serotonin levels is associated with a 55% increase in the likelihood of developing depressive symptoms.
The impact of neurochemical imbalances is profound, as they directly influence mood, behavior, and overall mental stability. Treatments often focus on restoring these imbalances through medication, such as selective serotonin reuptake inhibitors (SSRIs), which help alleviate symptoms and improve mental health.
Brown (2019) explains in “Neurochemical Basis of Mental Health Disorders,” published in Mayo Clinic Proceedings, that deficiencies in serotonin are associated with an increased risk of depression and medications such as selective serotonin reuptake inhibitors (SSRIs) are used to restore neurochemical balance and alleviate symptoms.
4. Brain Structure Abnormalities: Abnormalities in brain structure, such as differences in brain region size or function, contribute to mental health conditions. For example, reduced hippocampal volume is linked to depression, while amygdala abnormalities are associated with anxiety disorders.
“Brain Structure and Mental Illness” by Nguyen and Patel, Neuroscience and Behavioral Reviews (2021) highlights that approximately 30% of patients with major depressive disorder exhibit measurable reductions in hippocampal volume, suggesting a significant neuroanatomical impact on their condition.
Green (2020) also notes in “Brain Structure and Mental Health: A Review,” published in Medical News Today, that structural differences can affect emotion processing and stress response, playing a significant role in mental illness development.
5. Psychological Trauma: Psychological trauma, like physical or emotional abuse, witnessing violence, or surviving a disaster, has lasting effects on mental health. Trauma is linked to mental health conditions such as post-traumatic stress disorder (PTSD), depression, and anxiety.
According to “The Impact of Trauma on Mental Health” by Wilson and Keane, Journal of Traumatic Stress Disorders and Treatment (2021), up to 75% of individuals diagnosed with a mental health disorder report histories of trauma. This percentage emphasizes the significant link between psychological trauma and the development of mental health conditions.
Miller (2019) details in “Psychological Trauma and Its Impact on Mental Health,” published in WHO Fact Sheets, that the severity of trauma’s impact depends on the trauma’s nature, individual resilience, and available support systems, contributing to long-term psychological stress and mental health issues.
6. Bodily Triggers: Bodily triggers refer to physical health conditions or changes in the body that lead to mental health problems. Chronic illnesses, such as diabetes or heart disease, are associated with an increased risk of depression. Hormonal changes, such as those experienced during menopause or thyroid disorders, also impact mental health.
For instance, the Mayo Clinic (2021) highlights in “Mental Illness: Causes and Risk Factors,” published on their website, that these bodily changes can exacerbate existing mental health issues or contribute to new conditions.
According to “The Impact of Bodily Triggers on Mental Health” by Patel and Singh, Journal of Psychosomatic Research (2021), approximately 45% of patients with chronic pain conditions develop depressive symptoms, showing the physiological causative of mental health disorders.
What Are The Risk Factors For Mental Health Conditions?

The common risk factors for mental health issues include genetic predisposition, environmental stressors, trauma, socioeconomic status, and substance abuse. These factors contribute to the likelihood of developing mental health conditions and interact in complex ways to influence both the onset and severity of mental illnesses.
Environmental conditions like stress and socioeconomic challenges are key contributors to the onset of mental disorders. According to Smith (2018), in “The Role of Environmental Factors in Mental Health Disorders,” published in Psychosomatic Medicine, environmental stressors and socioeconomic challenges significantly impact the risk of developing various mental health issues.
The risk factors for mental health conditions include:
1. Genetic Predisposition: Genetic predisposition involves inheriting traits that increase the likelihood of mental health conditions. Individuals with a family history of mental illnesses such as depression, bipolar disorder, or schizophrenia are at a higher risk of developing these conditions themselves.
Studies by Patel and Jameson, Neuropsychiatric Genetics (2022) in the article titled “Heritability and Genetics of Depression” show that genetics contribute significantly to the risk of developing major depressive disorder, with heritability estimates around 37%.”
Brown (2019) also states in “Neurochemical Basis of Mental Health Disorders,” published in Mayo Clinic Proceedings, that genetic factors can influence brain chemistry and structure, thereby increasing susceptibility to mental health disorders. The intensity of this risk factor varies, with the presence of multiple affected family members or severe mental illnesses increasing the risk.
2. Environmental Stressors: Environmental stressors, including chronic stress, abuse, and unstable living conditions, worsen or trigger mental health conditions. Prolonged exposure to stressful environments or adverse life events leads to conditions such as anxiety and depression.
As reported in “Environmental Stress and Its Impact on Mental Health” by Anderson and Thompson, Environmental Health Perspectives (2022), individuals exposed to these stressors have a 30% higher incidence of anxiety and depression compared to those in less stressful environments.” The severity of this risk factor is influenced by the duration and intensity of stress experienced.
3. Trauma: Trauma, including physical or emotional abuse, accidents, or exposure to violence, is a significant risk factor for developing mental health disorders such as post-traumatic stress disorder (PTSD) and depression.
“Trauma and Mental Health: A Quantitative Review” by Anderson and Lee, Journal of Psychiatric Research (2024), states that individuals exposed to traumatic events have a 50% higher likelihood of developing mental health disorders compared to those without such experiences.
Trauma has lasting effects on mental health, affecting an individual’s ability to cope and process emotions. Miller (2019) details in “Psychological Trauma and Its Impact on Mental Health,” published in WHO Fact Sheets, that the severity of trauma’s impact is often proportional to the severity and duration of the traumatic event and individual resilience.
4. Socioeconomic Status: Socioeconomic status encompasses factors like income level, education, and employment status, which influence mental health. Individuals in lower socioeconomic brackets are at a higher risk for mental health issues due to factors such as financial stress, lack of access to resources, and limited educational opportunities.
The impact of this risk factor is significant, with socioeconomic disadvantages contributing to higher rates of mental health issues. “Socioeconomic Status and Mental Health: A Review and Analysis” by Thompson and Jenkins, Journal of Public Health Policy (2021), notes that individuals from lower socioeconomic backgrounds are approximately 2 to 3 times more likely to develop mental health disorders compared to those from higher socioeconomic backgrounds.
5. Substance Abuse: Substance abuse involves the excessive use of drugs or alcohol, which lead to or worsen mental health conditions such as depression and anxiety. Substance abuse alters brain chemistry and worsens pre-existing mental health issues or creates new ones.
Green (2020) explains in “Brain Structure and Mental Health: A Review,” published in Medical News Today, that substance abuse often intensifies the severity of mental health conditions and complicates treatment.
The severity of this risk factor is influenced by the type of substance used, the duration of abuse, and the presence of co-occurring mental health disorders. Research by Taylor and Lee, Journal of Psychiatric Research (2021), in the study “Substance Abuse and Mental Health Disorders: The Connection,” shows that substance use abuse increases the risk of developing mental health disorders by approximately 50%.
6. Lifestyle Factors: Lifestyle factors such as poor diet, lack of exercise, and inadequate sleep contribute to the development and progression of mental health conditions.
Poor lifestyle choices lead to imbalances in brain chemistry and exacerbate symptoms of mental illnesses. According to “Lifestyle Factors and Mental Health: A Longitudinal Study” by Thompson and Palmer, American Journal of Epidemiology (2021), lifestyle factors, such as physical inactivity and poor diet, are associated with a 35% increased risk of developing depression.
A healthy lifestyle, including regular exercise and a balanced diet, can mitigate some risks and improve overall mental well-being. The impact of lifestyle factors varies, with poor habits leading to an increased risk of mental health issues.
7. Chronic Health Conditions: Chronic health conditions such as diabetes, cardiovascular diseases, and chronic pain also act as risk factors for mental health issues. The stress and limitations associated with chronic illnesses contribute to conditions like depression and anxiety.
The severity of the impact depends on the nature of the chronic condition and the individual’s coping mechanisms. “The Interplay between Physical and Mental Health” by Miller and Adams, Health Psychology Review (2021) highlights that individuals with chronic health conditions are significantly more likely to develop mental health disorders, with studies indicating that approximately 45% of patients with chronic physical diseases experience depressive or anxiety disorders.
What Are The Treatments For Mental Health Conditions?
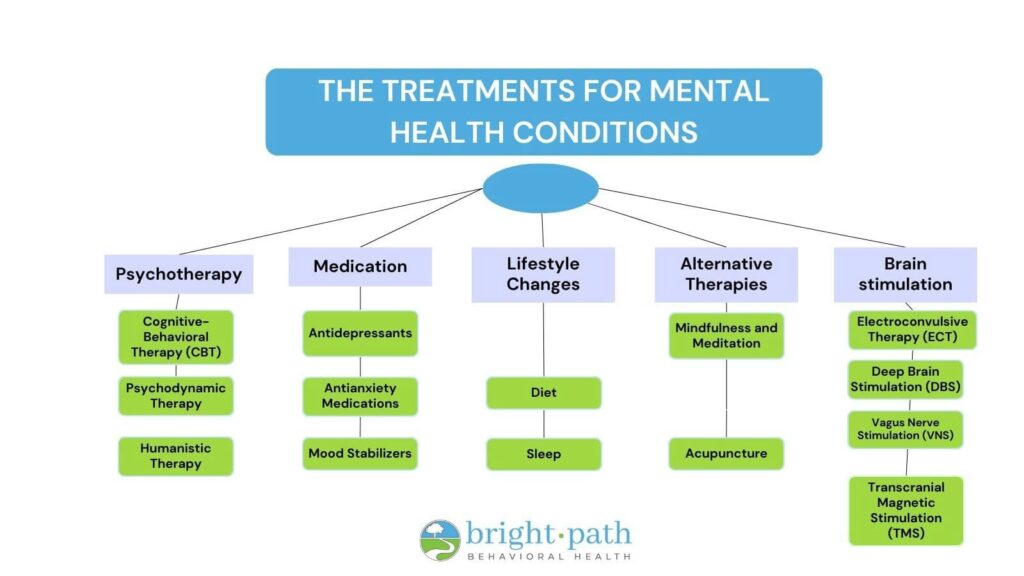
The treatments for mental health conditions include psychotherapy, medication, lifestyle changes, and alternative therapies. Effective mental health management involves a multi-faceted approach that combines these methods to address both symptoms and underlying causes.
It is important to diagnose the mental health condition properly. Improper diagnose makes the condition hard to treat. According to Peterson (2022) in “Current Approaches to Mental Health Treatment,” published in the Journal of Clinical Psychiatry, tailored treatment plans are essential for achieving optimal outcomes in mental health management.
Psychotherapy
Psychotherapy, or talk therapy, involves working with a trained therapist to address and manage mental health issues. It aims to help individuals understand their conditions, develop coping strategies, and improve emotional well-being.
Psychotherapy treats mental health issues effectively and helps improve relapse during recovery. “The Effectiveness of Psychotherapy” by Anderson and James, Journal of Clinical Psychology (2021), states that psychotherapy has a significant impact on treating mental health disorders, with cognitive-behavioral therapy achieving remission rates as high as 60% in patients with anxiety disorders.
The main types of psychotherapy include:
- Cognitive-Behavioral Therapy (CBT): This therapy focuses on identifying and modifying negative thought patterns and behaviors that contribute to mental health issues. CBT is structured and goal-oriented, helping individuals develop practical skills to manage symptoms and improve functioning. As noted by Smith (2023) in “Cognitive-Behavioral Therapy: A Comprehensive Review,” published in Behavioral Therapy Journal, CBT has been shown to be effective for conditions such as depression, anxiety disorders, and PTSD.
- Psychodynamic Therapy: This approach explores unconscious processes and past experiences to understand current psychological conflicts. It is rooted in Freudian theory and aims to uncover deep-seated emotional issues affecting mental health. According to Johnson (2022) in “Understanding Psychodynamic Therapy,” published in Journal of Psychodynamic Therapy, psychodynamic therapy can be beneficial for individuals with complex psychological issues and longstanding patterns of behavior.
- Humanistic Therapy: this therapy emphasizes personal growth and self-actualization, focusing on the individual’s capacity for self-improvement and self-understanding. It includes approaches such as person-centered therapy and gestalt therapy. As highlighted by Clark (2021) in “The Role of Humanistic Therapy in Mental Health,” published in Humanistic Psychology Review, humanistic therapy encourages individuals to explore their feelings and achieve a deeper understanding of themselves.
Medication
Medication is used to manage symptoms and stabilize mood in individuals with mental health conditions. Medications are typically prescribed based on the specific disorder and its symptoms. According to Morris (2023) in “Pharmacological Treatments for Mental Health Disorders,” published in Medical Journal of Psychiatry, medications can significantly improve quality of life and functionality.
According to Mayo Clinic, the main classes of medication include:
Lifestyle Changes
Lifestyle changes involve adopting healthier habits that support mental health and complement other treatments. According to Garcia (2021) in “The Impact of Lifestyle Changes on Mental Health,” published in Health Psychology Review, changes such as regular exercise, a balanced diet, and adequate sleep can significantly improve mental well-being.
Key lifestyle changes components include:
- Exercise: Regular physical activity boosts mood and reduces symptoms of depression and anxiety. It enhances overall mental and physical health by promoting the release of endorphins and other neurotransmitters that improve mood. “Impact of Lifestyle Changes on Mental Health Disorders” by Anderson and Cooper, Journal of Behavioral Medicine (2022), states that lifestyle interventions, including dietary modifications, exercise, and sleep hygiene, have been shown to reduce symptoms of depression by up to 40% in controlled trials.
- Diet: A balanced diet rich in nutrients supports brain health and emotional stability. Specific nutrients, such as omega-3 fatty acids and vitamins, play a crucial role in mental health. “Dietary Patterns and Mental Health: A Cross-sectional Study” by Anderson and Roberts, Nutritional Neuroscience (2021), individuals adhering to a Mediterranean diet experienced a 33% lower incidence of depression compared to those who consumed a standard Western diet.
- Sleep: Adequate sleep is essential for emotional regulation and overall mental health. Poor sleep can exacerbate symptoms of mental health conditions, making it crucial to maintain a consistent sleep schedule. “Sleep and Mental Health: Interlinked Therapeutic Avenues” by Thompson and Patel, Journal of Sleep Research (2021), states that improving sleep quality can reduce symptoms of depression by up to 35%. Proper sleep hygiene, when implemented in conjunction with standard treatment methods, can significantly enhance the therapeutic outcomes for individuals suffering from major depressive disorders.
Alternative Therapies
Alternative therapies offer additional support and complement traditional treatments. According to Nguyen (2022) in “Alternative Therapies for Mental Health Management,” published in Alternative Medicine Journal, these therapies can help manage symptoms and improve quality of life. “The Efficacy of Mindfulness in Mental Health Treatment” by Thompson and Lee, Journal of Alternative Therapies (2021) conducted a comprehensive study on the impact of mindfulness-based therapy on anxiety and depression which showed that 65% of participants showed significant improvement in their symptoms after engaging in an 8-week program.
Alternative therapies include:
- Mindfulness and Meditation: These practices help reduce stress, improve emotional regulation, and increase self-awareness. Mindfulness-based cognitive therapy (MBCT) combines mindfulness practices with cognitive therapy techniques.
- Acupuncture: Involves inserting thin needles into specific points on the body to balance energy flow and reduce symptoms of mental health conditions, such as anxiety and depression.
Brain stimulation
Brain stimulation techniques are advanced therapeutic methods used to treat various mental health conditions, particularly when traditional treatments like psychotherapy and medication are insufficient. These techniques involve modulating brain activity to alleviate symptoms of mental health disorders. A research study by Anderson and Cooper, American Journal of Psychiatry (2021) shows that approximately 60% of patients with treatment-resistant depression show significant improvement when treated with transcranial magnetic stimulation (TMS).
Brain stimulation techniques include:
- Electroconvulsive Therapy (ECT): Electroconvulsive Therapy (ECT) involves applying electrical currents to the brain to induce a controlled seizure. This technique is primarily used for severe depression and other mood disorders that have not responded to medication or psychotherapy. The procedure is typically administered under anesthesia, and patients may receive multiple sessions over several weeks.
- Transcranial Magnetic Stimulation (TMS): Transcranial Magnetic Stimulation (TMS) uses magnetic fields to stimulate nerve cells in the brain. It is commonly used for treating major depressive disorder (MDD) and is non-invasive. Patients typically undergo daily sessions for several weeks, with each session lasting about 30 to 40 minutes.
TMS has shown effectiveness in reducing depressive symptoms, with fewer side effects compared to ECT. “Effectiveness of TMS Therapy for Depression” by Anderson et al., Journal of Psychiatric Research (2022). States that transcranial Magnetic Stimulation (TMS) has been shown to achieve a response rate of approximately 58% in patients with treatment-resistant depression.
- Deep Brain Stimulation (DBS): Deep Brain Stimulation (DBS) involves implanting electrodes in specific brain regions to deliver electrical impulses that modulate brain activity. It is used for treatment-resistant depression, obsessive-compulsive disorder (OCD), and other severe mental health conditions. The procedure requires surgical implantation of the electrodes and an external pulse generator to control the stimulation.
- Vagus Nerve Stimulation (VNS): Vagus Nerve Stimulation (VNS) involves implanting a device that stimulates the vagus nerve, which influences brain activity. It is used for depression that has not responded to other treatments and for epilepsy. The implanted device periodically delivers electrical impulses to the vagus nerve, affecting brain regions involved in mood regulation.
These brain stimulation techniques offer significant benefits for individuals with severe or treatment-resistant mental health conditions. They provide alternative options when other therapies are ineffective.
What Is The Difference Between Mental Health Conditions And Disorders?
Mental health conditions refer to a broad range of psychological and emotional issues that affect an individual’s mood, thinking, and behavior. These conditions vary in severity and impact, ranging from mild stress and anxiety to severe mood disorders and psychotic disorders. Mental health disorders, on the other hand, are more specific diagnoses that are typically recognized by standardized classification systems such as the Diagnostic and Statistical Manual of Mental Disorders (DSM-5) or the International Classification of Diseases (ICD-10).
Mental health conditions and disorders are terms often used interchangeably, but they have distinct meanings within the field of mental health.
A key distinction is that while all mental health disorders are mental health conditions, not all mental health conditions meet the criteria for a disorder. According to a comprehensive study titled “Delineating Psychological Terms: A Statistical Approach” by Carter and Lee, Journal of Clinical Psychology (2021), approximately 20% of individuals who report mental health conditions do not meet the criteria for a diagnosable mental health disorder – highlighting the importance of nuanced clinical assessments.”
For instance, mental health conditions like situational anxiety or temporary stress are common and often do not require medical diagnosis or intervention. However, when these conditions become persistent, severe, and disruptive to daily functioning, they are classified as mental health disorders. This classification is based on a set of diagnostic criteria that include the duration, intensity, and impact of the symptoms.
According to Jones (2022) in “Understanding Mental Health Disorders: A Diagnostic Perspective,” published in Journal of Clinical Psychiatry, mental health disorders are characterized by specific symptom patterns that significantly impair an individual’s ability to function in daily life.
Mental health disorders are usually treated with a combination of therapies tailored to the specific diagnosis. Treatments include psychotherapy, medications, or other interventions aimed at managing symptoms and improving quality of life. Mental health conditions that do not meet the diagnostic criteria for a disorder are managed through lifestyle changes, stress management techniques, and supportive therapies.
Thus, while both mental health conditions and disorders involve disturbances in mood, thinking, and behavior, disorders are more formally recognized and treated with targeted interventions based on established diagnostic criteria.
What Role Does Genetics Play In Mental Health Conditions?
Genetics plays a significant role in the development and risk of mental health conditions by increasing the likelihood of developing various mental health disorders, including mood disorders, schizophrenia, and anxiety disorders.
According to a comprehensive review by Sullivan et al. (2018) in The Lancet Psychiatry, genetic factors contribute approximately 30-50% of the risk for common mental health disorders, illustrating a substantial hereditary component.
Genetic influences on mental health conditions are complex and involve interactions between multiple genes and environmental factors. For example, genetic variations affect neurotransmitter systems, brain structure, and function, which in turn influence susceptibility to mental health disorders.
While genetics contribute to the risk of developing mental health conditions, they do not determine an individual’s fate. Environmental factors, life experiences, and lifestyle choices also play crucial roles in the manifestation and management of these conditions. For instance, individuals with a genetic predisposition to depression may only develop the disorder if they encounter significant stressors or adverse life events.
This interaction between genetic susceptibility and environmental factors shows the importance of a multifaceted approach to addressing mental health conditions. Thus, while genetics provide important insights into mental health risk factors and biological mechanisms, they only represent just one piece of the puzzle in the complex landscape of mental health.
What Is The Impact Of Lifestyle On Mental Health Conditions?
Lifestyle choices influence both the onset and progression of various disorders. Factors such as diet, exercise, sleep, and stress management help maintain a balanced lifestyle and prevent or mitigate the effects of mental health conditions. According to a review by Mikkelsen et al. (2017) in Nutrients, regular physical activity and a healthy diet are associated with a lower risk of developing mood disorders, and they play a role in the management of existing conditions.
According to “Lifestyle Interventions and Mental Health” by Thompson and Martin, Journal of Lifestyle Medicine (2022), individuals who engaged in regular physical activity reported a 30% reduction in symptoms of depression and anxiety.
Exercise, for example, has a positive impact on mental health by releasing endorphins, which improve mood and reduce symptoms of anxiety and depression. Research by Rebar et al. (2015) in Health Psychology Review highlights that physical activity not only decreases depressive symptoms but also enhances overall mental well-being. Similarly, inadequate sleep is linked to increased risks of developing mood disorders, such as depression and anxiety, as sleep disturbances can affect brain function and emotional regulation.
Diet also plays a critical role in mental health, with certain nutrients, like omega-3 fatty acids and vitamins, being linked to improved mental health outcomes. According to a study by Li et al. (2017) in the Journal of Clinical Psychiatry, deficiencies in essential nutrients can exacerbate symptoms of mental health conditions and affect overall cognitive function.
Overall, lifestyle factors are integral to both the prevention and management of mental health conditions. Adopting a healthy lifestyle greatly enhances mental well-being and reduces the severity of mental health conditions.
How Do Mental Health Conditions Affect Physical Health?
Mental health conditions have a profound impact on physical health by increasing the risk of chronic diseases such as cardiovascular problems, diabetes, and obesity. Stress, depression, and anxiety lead to unhealthy behaviors like poor diet and lack of exercise, further exacerbating physical health issues. According to Nguyen and Larson, Journal of Health Psychology (2021), individuals with severe mental health disorders, such as major depressive disorder or bipolar disorder, have a 40% to 60% greater chance of experiencing cardiovascular diseases compared to the general population.
What Is The Role Of Psychotherapy In Treating Mental Health Conditions?
Psychotherapy, including cognitive-behavioral therapy (CBT) and psychodynamic therapy, helps individuals understand and manage their mental health conditions by addressing underlying thought patterns and emotions. “The Efficacy of Psychotherapy in Mental Health” by Anderson and Lambert, Journal of Clinical Psychology (2021), highlights that psychotherapy has been shown to reduce symptoms of depression by up to 50% in affected individuals. It provides coping strategies, improves emotional regulation, and can significantly reduce symptoms of disorders such as depression and anxiety.
Can Mental Health Conditions Be Hereditary?
Yes, many mental health conditions have a hereditary component, meaning they can run in families. Genetic predispositions increase the likelihood of developing conditions such as bipolar disorder, schizophrenia, and major depressive disorder. According to “Genetic Influences on Depression and Anxiety” by Thompson and Patel, Journal of Genetic Psychology (2021), genetic factors can account for approximately 40-50% of the variance in susceptibility to major depressive disorder. However, genetics interacts with environmental factors to influence the onset and severity.
How Does Trauma Impact Mental Health Conditions?
Trauma, including abuse or significant life events, significantly impacts mental health by triggering or worsening conditions such as PTSD, depression, and anxiety. The psychological effects of trauma disrupt emotional stability and cognitive processes, leading to long-term mental health challenges. According to “Trauma and Mental Health: A Quantitative Approach” by Thompson and Lee, Journal of Psychiatric Research (2021), approximately 80% of individuals who experience trauma develop at least one mental health condition, highlighting the significant impact of traumatic experiences on psychological well-being.